The Liability Risks Hidden in Your Employee Benefits Data

Conference Board of Canada: "Employee benefits could not be more important to engagement and retention of an organization's workforce - or, in many cases, more misunderstood."
Administering even simple employee benefit plans can be complex and time consuming, and even simple administration errors or omissions can expose your organization to significant liability. These issues only get worse if you want to take advantage of leveraging multiple carriers in order to construct a best-in-class benefits plan.
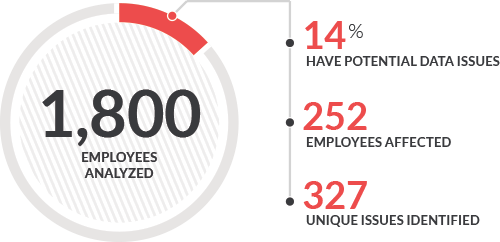
Our research and experience finds that on average 14% of employee data administered directly with insurance carriers or through traditional third party administration providers has errors in it. These errors can be difficult to identify and can pose serious liabilities to your organization. For example, common errors include:
- Missed enrollments resulting in no coverage and a possible reduction or denial of coverage when discovered
- Missed terminations resulting in inappropriate plan utilization and the risk of increased rates
- Incorrect disability benefit volumes which can result in millions of dollars of liability and associated legal fees
- And many more...
Consider the following case study:
Mr. Bennet is a 35 year old male who was recently employed with ABC Company. Due to a simple administrative data entry error, he was not enrolled in the company benefits plan. A year later Mr. Bennet was in an accident and became disabled. His application for the long term disability benefit however, was denied.
At the time of his disability Mr. Bennet was earning $75,000 annually. If he remains disabled until the benefit termination age of 65 ABC Company may be liable up to a maximum of $1,500,750 in disability payout based on the benefit provisions in his policy.
This is only one of many examples of significant liabilities that can easily exist in your eligibility data.
Given the likelihood that many of these issues exist in your current benefit plan administration data...
- How do you identify the types of issues that might exists?
- How do you approach a data audit in a thorough way?
- How do you prevent these liabilities from occurring in the future?
Performing a manual administration data audit is a big commitment and a time consuming process. Even with good processes in place this type of audit should be performed on a routine basis and quickly becomes too burdensome. However to do so manually, each line of benefit for each employee needs to be reviewed and confirmed by cross referencing the system data of the carrier supporting that line of benefit with the relevant provisions of that carrier’s administration guide and policy contract provisions for that line of benefit, and this information must also be compared against the company’s payroll and HRIS data to ensure proper class / division allocation and volume calculations.
So how can you stay on top of the integrity of your data in a way that doesn’t break the bank?
Effortless Admin specializes in performing benefits administration data audits that expose many of the contract compliance issues cited above. On average, we find that 14% of employees have some form of obvious inaccuracy in their data.

The majority of these data issues are corrected automatically when administering an employee benefits plan through the Effortless Admin platform due to its industry leading rules based architecture. Not only does this help improve the accuracy of employee data at the time of enrollment but it greatly improves data accuracy over time.
Going one step further and taking advantage of one of our payroll or HRIS integrations will also help reduce data transposition errors by removing any duplicate data entry required between your payroll/HRIS system and the Effortless Admin platform.
Talk to us about us about how we can help reduce your liability.